“The desire to avoid unnecessary interventions during labor and birth is shared by health care providers and pregnant women. Obstetricians-gynecologists, in collaboration with midwives, nurses, patients, and those who support them in labor, can help women meet their goals for labor and birth by using techniques that require minimal interventions and have high rates of patient satisfaction.”
In their recently updated (February 2019), evidence-based Committee Opinion, Approaches to Limit Intervention During Labor and Birth, the American College of Obstetrics and Gynecology (ACOG) recommends that “caregivers should be familiar with and consider using low-interventions for low-risk women who go into labor on their own.” ACOG affirms that many commonly used obstetric practices are of limited or uncertain benefit for low-risk women who go into labor on their own.
For women with a single fetus in a head-down position who go into labor on their own at term (37 to 41 0/7 weeks) and do not experience complications, “providers should carefully select and tailor labor interventions to meet safety requirements and the individual woman’s preference.”
The ACOG recommendations to limit interventions reflect many components of midwifery care and are endorsed by the American College of Nurse-Midwives (ACNM).
Approaches to Limit Intervention During Labor and Birth (Committee Opinion Number 766) encourages the following low-intervention practices.
- Premature Rupture of the Membranes at Term (PROM)
A woman should be given the choice to wait until labor begins or be induced after having been given information about the benefits and risks of each option unless she is GBS positive (Group B Strep). Many caregivers recommend that labor be induced soon after the bag of waters has broken (amniotomy) although most women will go into labor within 12 to 24 hours.
- Admission to the Birthing Unit
Admission to the birthing unit may be delayed for women in latent labor (before 5-6cm of dilation) if their vital signs are stable and the status of the fetus is reassuring.
Women admitted to a birthing unit in early labor have higher rates of labor augmentations and epidurals. They spend more time in labor and delivery and are less satisfied with their birth. At prenatal visits, women and their caregivers should discuss a personal plan for self-care, early labor pain coping techniques, and activities to help them at home or in an early-labor lounge, until formally admitted to the labor unit. While laboring at home, women can benefit from frequent contact and support from their caregivers.
- Routine Interventions
In the absence of medical complications, women do not need routine continuous electronic fetal monitoring (EFM) or a continuous IV infusion. Caregivers should be trained to use a hand-held Doppler for intermittent auscultation for women who wish to have this option during labor. Continuous EFM does not significantly affect perinatal death or cerebral palsy when used for women with a low-risk pregnancy but does increase the odds for a cesarean and instrumental delivery when compared with intermittent monitoring.
When labor is progressing normally many caregivers routinely break the bag of waters to “speed up labor.” Evidence shows that the procedure does not make much difference nor does it lower the risk for a cesarean.
- Non-drug Methods for Coping with Labor
Women should be free to drink (clear liquids) during labor and use any of the following options that meet their needs; water immersion, massage, relaxation and breathing techniques, acupuncture, sterile water injections, TENS (transcutaneous electrical nerve stimulation), aromatherapy and audio analgesia.
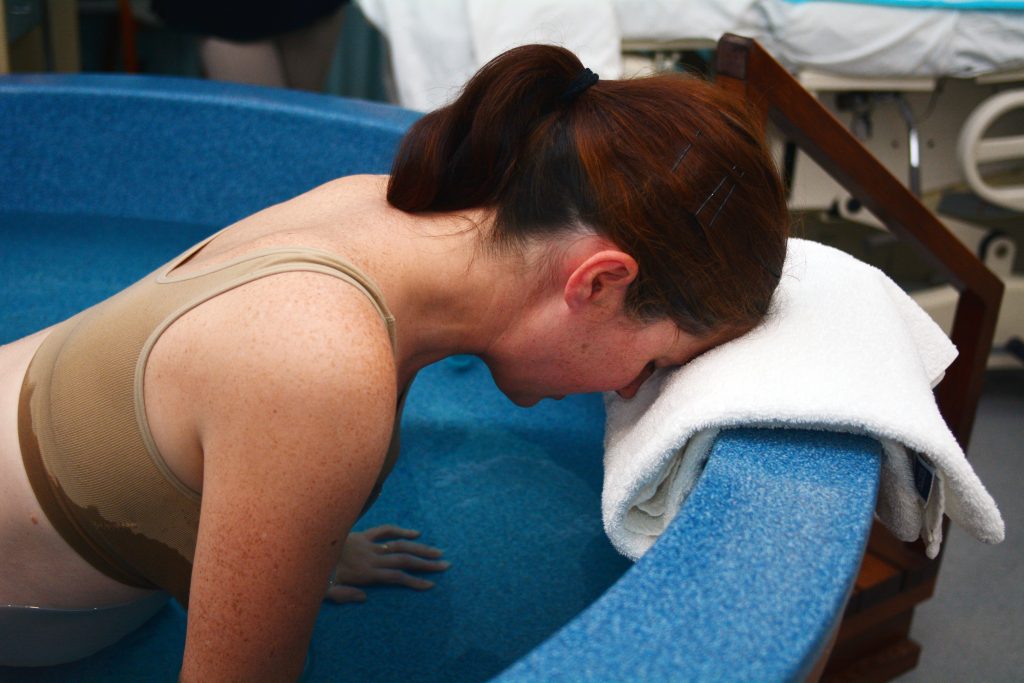
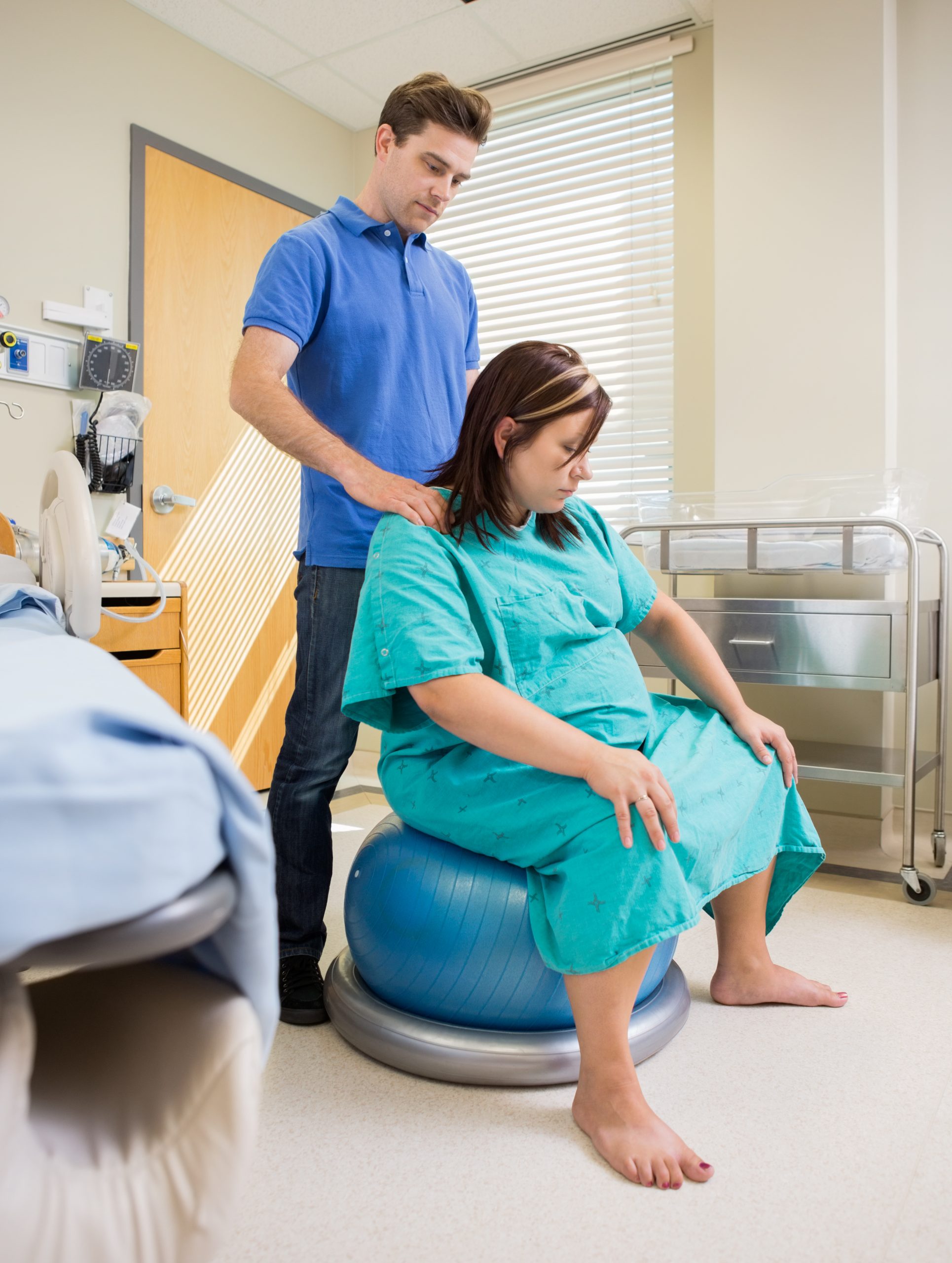
- Positions in Labor and Birth
Women should be encouraged to use any comfortable upright position in labor such as walking, sitting, standing, or kneeling. Compared to laboring on the back, upright positions reduce the risk for maternal hypotension and abnormal fetal heart rate. By using upright positions women can shorten their labor by about 1 hour and 22 minutes and they are less likely to end up with a cesarean.
For women who choose an epidural for pain relief in labor the evidence suggests that women push at the start of the second stage of labor. With an epidural delayed pushing increases the odds for maternal infection, hemorrhage, and neonatal acidemia.

- Pushing in Second Stage
Women should not be restricted to any specific breathing or pushing method for second stage. They should be supported in their own choice of breathing patterns and pushing positions that work best for them.
- Support in Labor
In addition to nursing care, continuous one-to-one emotional and physical support provided by non-medical experienced personnel such as a doula is associated with improved outcomes for women and babies. Labor is shorter, women are less likely to use drugs for pain relief and less likely to have a cesarean. Babies tend to have a higher Apgar score and are more likely to establish successful breastfeeding. Overall mothers are more satisfied with their birth experience.
Hospitals are encouraged to integrate trained support personnel in their maternity care staff.

- Family-centered Birth
For both vaginal and cesarean births, women value the presence and support of family members. Whenever possible, hospitals are encouraged to integrate family-focused practices for cesarean births such us lowering the drapes or using surgical drapes with a viewing window for parents to see the birth of their baby, lowering the lights, reducing extraneous noise, adding music, delayed cord-clamping, and skin-to-skin attachment of mother and newborn.
It’s worth noting that these guidelines to avoid unnecessary interventions are the most comprehensive to date. They also endorse women’s freedom to choose how they want to give birth.
Revised March 10, 2019




0 Comments